
If You Want to Go Far, Go Together
Takeaways from the Delta Center Convening #6
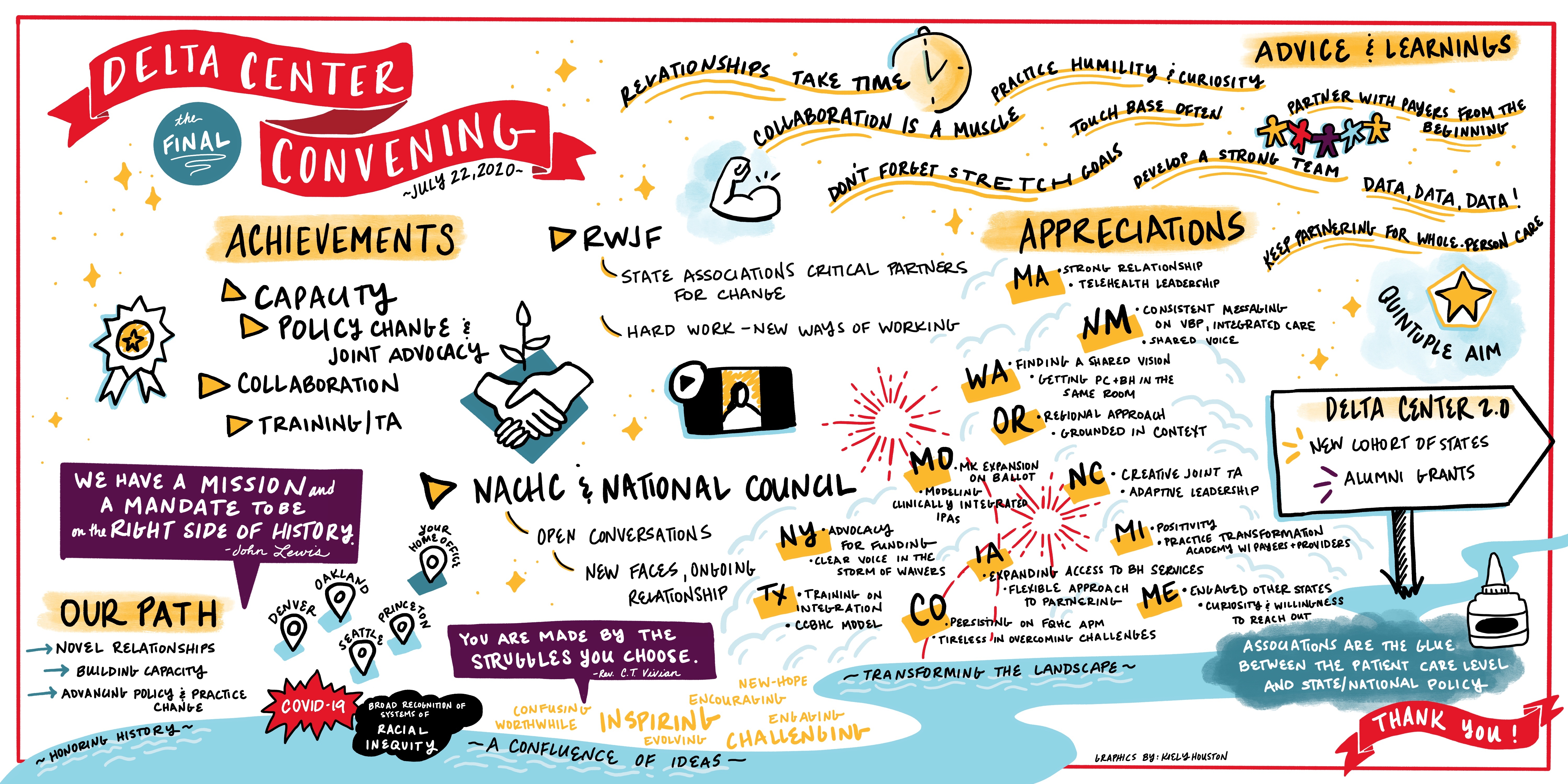
The Delta Center for a Thriving Safety Net held a sixth and final convening virtually on July 22, 2020. This occasion allowed us to honor, recognize, and reflect on the Delta Center journey over the past two years. Grantees and coaches highlighted state teams’ accomplishments, shared learnings, and reflected on how goals had shifted in the wake of a novel public health emergency.
Amid the concurrent challenges of COVID-19 and a nationwide reckoning with the deep impacts of systemic racism, Delta Center grantees shared that their journey has not always been smooth. At the same time, grantees reflected that turbulence can also be a catalyst for meaningful change. Grantees shared how recent events had brought policy and practice together in accelerated fashion, exemplified in the rapid implementation of and payment for telehealth across all states. They also reflected that they were able to leverage experiences building partnerships to both shape and advance policy goals, illustrated by a ballot measure for Medicaid expansion in Missouri.
Rachel Tobey, co-director of the Delta Center, opened the convening with a look back on our journey, beginning from the June 2018 kickoff in Denver, CO, where grantees began to foster new relationships with their counterpart behavioral health (BHSA) or state primary care association (PCA). The Delta Center launched with three overarching goals building towards one core intention: building the internal capacity of behavioral health and primary care state organizations representing providers, a key part of the national safety-net infrastructure:
- Build policy and advocacy capacity to advance value-based payment and care (VBP/C) at the state level;
- Foster collaboration between primary care and behavioral health at the state level;
- Build capacity to provide TA and training on value-based payment and care at the provider level.
Over the past two years, grantees made meaningful progress towards all three of these goals. They shared their learnings and successes with the cohort during small group breakouts. Below, we highlight the main themes of the small group discussions which included individuals from grantee teams, RWJF, and Delta Center partners (MacColl, CCI, NACHC and NCBH).
What are you most proud of from your time in the Delta Center?
"We went from sometimes working at cross-purposes to a relationship that was BEDROCK in terms of mutual trust and the habit of pulling each other into policy conversations."
- Delta Center Grantee
- Strengthening relationships with their counterparts: Grantees highly valued their development of stronger and more enduring partnerships with their counterpart PCA or BHSA. They emphasized that these partnerships have brought new ideas and new energy to their efforts to shape both policy and practice. Previous to their Delta Center collaboration, several associations had experienced a weak or even nonexistent relationship with their counterpart; in some cases, grantees even characterized prior relationships as being competitive. The Delta Center created an opportunity for associations to align on a set of goals and meaningfully collaborate to pursue them. When the COVID-19 crisis hit, grantees were poised to leverage these relationships and respond to the needs of their members, and, ultimately, patients/consumers served by health centers and community behavioral health organizations. The pandemic required the associations to pivot quickly in order to support their members in implementing telehealth. Grantees rose to the occasion, sharing lessons learned and advocating together to sustain telehealth beyond the pandemic. For example, the relationship between the state associations in Washington blossomed through the Delta Center; as the COVID-19 crisis emerged, they quickly came together to address gaps in telehealth policy. In Massachusetts, both associations aligned their approaches and participated on joint committees to identify areas for advocacy and best practices for rapidly-expanding telehealth. The associations in Missouri both advocated for a critical policy change that would expand access to both behavioral health and physical health care: Medicaid expansion (which ended up passing in a ballot measure a few weeks later). Regular collaboration provided more opportunity for associations to stay attuned to each other’s goals, tap into each other’s work, and be regarded as a collective voice.
“The state now thinks of us as a partner and not opposition, and during COVID has looked to us to help guide them.”
- Delta Center Grantee
- Collaborating with state leaders: Many grantees also engaged in meaningful collaboration with state policymakers, including legislators and Medicaid leaders; this enabled joint efforts between primary care and behavioral health on advocacy, training, and policy work. For example, New Mexico had a strong focus on building relationships with state policymakers, agencies, payers, and providers. They worked to bridge gaps in knowledge around care integration and value-based payment and care (VBP/C) at statewide convenings. New York authored a telehealth paper that argued for making the vast flexibilities temporarily granted to behavioral health and FQHC providers permanent. The paper has garnered attention from policymakers in the state. In North Carolina, a collaborative of managed care organizations, behavioral health organizations, the North Carolina Department of Health & Human Services, and the PCA emerged to look at an alternative payment methodology related to community support teams. These efforts all illustrate how the Delta Center provided a foundation from which associations are continuing to strengthen policy around their goals.
- Building momentum around value-based payment and care: In multi-level collaboration efforts with their state counterparts and association members, grantees developed strategies around VBP/C and creating a more unified safety net, and then spread these developments through their networks. For example, Michigan conducted a Practice Transformation Academy with their members, resulting in 28 members developing alternative payment model approaches. Maine increased outreach to both primary care and behavioral health members within the state and conducted a series of trainings around VBP/C. In Oregon, the associations strengthened mental health parity in their state. Associations in Iowa developed a capitation APM. Despite encountering multiple challenges, Colorado celebrated the launch of its second FQHC APM structure. Texas achieved system-wide support from all 39 members for the Certified Community Behavioral Health Clinic (CCBHC) model of care and agreed upon a standardized population-based payment strategy.
What was your biggest learning?
- Buy-in from payers is critical: Grantees emphasized the necessity of engaging payers early on in order to move forward with value-based payment and care. Further, mere dialogue with payers was insufficient. A sense of shared commitment to action was also necessary, whether through dedicated resources or contractual commitments by Medicaid agencies, in order to affect statewide change. To this end, grantees found it important to prioritize their organizational relationship with the state Medicaid agency and Medicaid managed care plans. They found that having a clear vision for how to apply VBP/C, along with data (it’s always about data!), were essential to fostering buy-in and making progress.
- Collaboration is a journey: Collaboration can be a long and bumpy road. Grantees often found that the systems between primary care and behavioral health, including business models and payment structures, differed significantly. Despite behavioral health and primary care having similar goals and serving the same populations, understanding the complexities of each other’s systems required lengthy discussion. Further, because neither field can do everything, partnership is necessary to achieve whole-person care. Grantees found the best successes when they invested time in frank, collegial, and frequent dialogues with their partners and counterparts. With this strong foundation, grantees were better able to navigate challenges and uncertainty as they worked to define common goals and priorities. In addition to short-term goals, they also found that having joint ‘stretch goals’ in place helped them to take advantage when unforeseen opportunities arose. The time invested in building these partnerships positioned grantees to adjust their goals in response to a changing environment: one participant summarized their journey as, “Pivot, pivot, pivot!”
“Collaboration is a muscle - the more you exercise it, the easier it gets.”
- Delta Center Grantee
We ended the meeting with coaches conducting a twelve-state salute, celebrating the work of grantees from each state and creating spaces for individuals to showcase and appreciate their mentors, colleagues, and collaborators.
During the virtual convening, we presented our vision for a Delta Center for a Thriving Safety Net 2.0. On August 15, RWJF approved a Phase 2 of the Delta Center, which will include eight alumni grants as well as eight new state association grantees that will be awarded in early 2021.

“This [work] is the lifeblood of how the system will survive going forward.”
- Delta Center Grantee